The purpose of this notice is to inform you of the type of information that the surgery holds; how that information is used; who we may share that information with; and how we keep it secure and confidential.
The surgery has a duty to ensure that your personal data is kept confidential, secure and used appropriately.
We are registered with the Information Commissioner’s Office as a Data Controller and our registration number is Z4729790.
What kind of information do we use?
There are different types of information collected and used across the NHS. It should be noted that information which cannot identify an individual does not come under the Data Protection Act 2018.
We use the following types of information/data:
- Anonymised data, which is data about you but from which you cannot be personally identified
- De-identified data with pseudonym identifier, which is data about you but we are able to track you through the patient pathway without using your personal information, and you cannot be personally identified
- De-identified data with weakly pseudonym identifier such as the NHS number. We use this to link two or more types of datasets together using your NHS number
- Personal data which you can be personally identified from (this includes information such as your name and address)
- Special category data which tells us something about you (this includes information such as your ethnicity and health information)
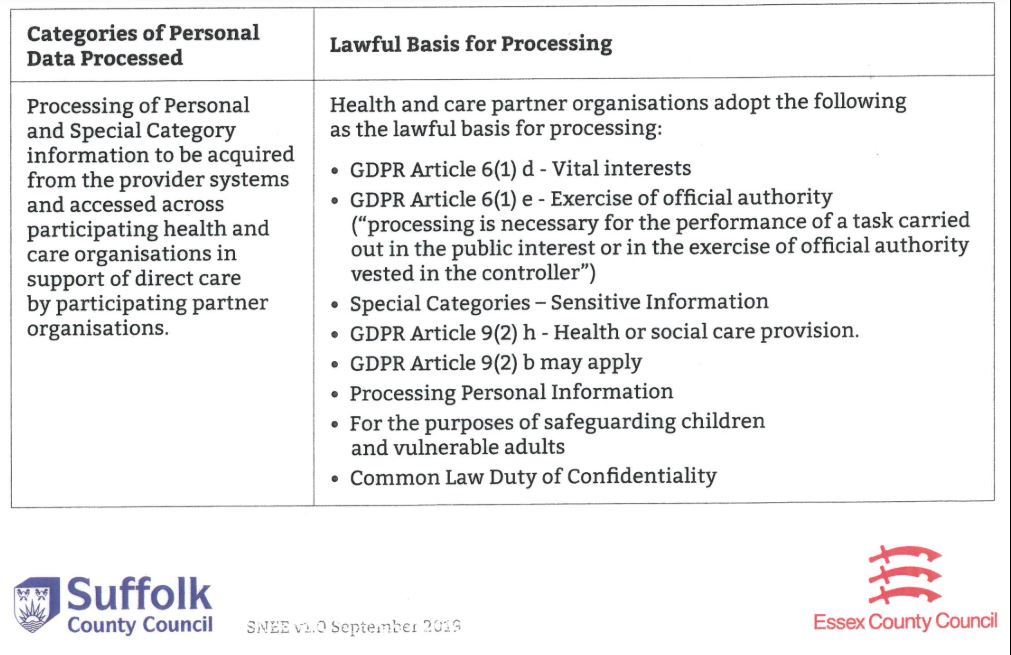
We will only use information that may identify you (known also as personal confidential data) in accordance with the: Data Protection Act 2018 – The Data Protection Act requires us to have a legal basis if we wish to process any personal information.
What do we use your information for?
We hold your medical record so that we can provide you with safe care and treatment. We will also use your information so that our surgery can check and review the quality of care we provide, this helps us to improve the service we provide to you. We shall share relevant information from your medical record with other health or social care staff or organisations when they provide you with care. For example, your GP will share information when they refer you to a specialist in hospital or your GP will send details about your prescription to your chosen pharmacy.
Aside from sharing information directly for your care, there are some other purposes that we may share data for, including:
Risk Stratification
Risk stratification is a process GPs use to help them to identify a person who may benefit from a targeted healthcare intervention and to help prevent un-planned hospital admissions or reduced the risk of certain diseases developing such as type 2 diabetes. This is called risk stratification for case-finding. As part of this, our surgery uses a primary care software system called Eclipse.
NHS Digital
NHS Digital is a national body which has legal responsibilities to collect information about health and social care services. It collects information from across the NHS in England and provides reports on how the NHS is performing. These reports help to plan and improve services to patients. This surgery must comply with the law and will send data to NHS Digital, for example, when it is told to do so by the Secretary of State for Health or NHS England under the Health and Social Care Act 2012.
The General Practice Extraction Service (GPES) collects information for a wide range of purposes, including providing GP payments. It works with the Calculating Quality Reporting Service (CQRS) and GP clinical systems as part of the GP Collections service. Find out more here.
Care Quality Commission (CQC)
The CQC regulates health and social care services to ensure that safe care is provided. The law says that we must report certain serious events to the CQC, for example, when patient safety has been put at risk. For more information about the CQC see: http://www.cqc.org.uk/
Public Health
The law requires us to share data for public health reasons, for example to prevent the spread of infectious diseases or other diseases which threaten the health of the population. We will report the relevant information to local health protection team or Public Health England.
Who do we share your information with?
We may share your information with other parties dealing with your care. When we do this we will inform you first unless we have a legal basis. We will not share your information with marketing organisations or other organisations that could cause you harm or lead to intrusive contact.
Some examples are:
- Local Council
- Hospital
- Mental Health Trust
- Ambulance Service
- Care Homes
- Social Care
- Safeguarding
- Suffolk and North East Essex Integrated Care Board (SNEEICB)
- Clinical system providers
- Police
- Coroner
- Confidential Waste removal company
- Voluntary Sector Organisations
We will keep you informed of how your data is used through this privacy notice, however please note that there may be times when we may not notify you such as for the prevention and detection of crime, safeguarding purposes, or as requested by a Court Order. We will only do this when the law requires us to do so.
Primary Care Network
We are a member of Deben South Primary Care Network (PCN). This means we will be working closely with a number of other Practices and health and care organisations to provide healthcare services to you.
During the course of our work we may share your information with these Practices and health care organisations/professionals. We will only share this information where it relates to your direct healthcare needs.
When we do this, we will always ensure that appropriate agreements are in place to protect your information and keep it safe and secure. This is also what the Law requires us to do.
If you would like to see the information the PCN holds about you please contact the Practice Manager. See also your rights as a patient listed below.
Multi-disciplinary Meetings
A multidisciplinary team (MDT) is a group of health and care staff who are members of different organisations and professions (e.g. GPs, social workers, nurses), that work together to make decisions regarding the treatment of individual patients and service users. MDTs are used in both health and care settings.
A list of MDT professionals could include the following:
Nurse Assessors, Social Care Practitioners, Physiotherapists, Occupational Therapist, Ward Nurses, Dieticians/Nutritionist, GPs/Consultants/Other Medical Practitioners, Community Psychiatric Nurses, Care Home/Support Provider Staff, Community Nurses, Specialist Nurses, Community Matrons and Discharge Nurses
MDT In Person vs Virtual
MDTs in their current format necessitate face-to-face contact between multiple clinical teams, they have the potential to act as potent accelerators of viral transmission. This created an urgent need to increase remote working across the health and care system. Teams are enabled to set Virtual MDTs using MS Teams which has given NHS staff a secure tool for instant messaging, video conferencing, sharing clinical information, images, and more
In an MDT, only information that is relevant and necessary for the patient or service user’s care will be shared.
Social Prescribing
Social Prescribing enables GPs, nurses and other primary care professionals to refer people to a range of local, non-clinical services. NHS England describes social prescribing as “enabling all local agencies to refer people to a link worker”. Link workers - known locally as Community Connectors - give people time and focus on what matters to the person. They connect people to community groups and agencies for practical and emotional support. If you have an appointment with a Community Connector, only limited information would be passed on. There are agreements in place to protect your data.
Diabetic Eye Screening
The Diabetic Eye Screening Programme in this area is provided by Health Intelligence after they were awarded the contract by NHS England Midlands and East to continue provision of the service from 1 April 2016. All patients aged 12 and over, with a diagnosis of diabetes will be referred by their GP surgery to the diabetic eye screening programme. You can find more information about this service as www.eadesp.co.uk
Text Messages
Please note that we will use your mobile number to text you with information regarding your care such as appointment reminders, flu vaccine booking etc. Please let us know if you would not like your mobile number used for this purpose.
Call Recording
Please note that this practice records its calls for training and quality purposes.
ROSI
The ROSI (Record Once Share Insight) solution is being developed for use across Suffolk and North East Essex Integrated Care System.
ROSI is an Advance Care Plan Electronic Record and will replace current documentation such as My Care Wishes in Suffolk. The record holds key information about patients, including their cardiopulmonary resuscitation (CPR) decision, language, family carers, capacity, their end-of-life preferences.
Please find the privacy notice for ROSI here.
How do we keep your information safe?
All staff have contractual obligations of confidentiality, enforceable through disciplinary procedures. All staff will receive appropriate training on confidentiality of information and staff who have regular access to personal confidential data will have received additional specialist training.
We take relevant organisational and technical measures to make sure that the information we hold is secure – such as holding information in secure locations, restricting access to information to authorised personnel, protecting personal and confidential information held on equipment such as laptops with encryption and information is transferred safely and securely.
The surgery does not transfer personal confidential information overseas without adequate protection.
Under the Data Protection Act 2018, the surgery is required to register with the Information Commissioner’s Office detailing all purposes for which personal identifiable data is collected, held and processed.
The surgery has a legal duty to protect any information we collect from you. We use leading technologies and encryption software to safeguard your data and keep strict security standards to prevent any unauthorised access to it.
The surgery will not pass on your details to any third party or other government department unless you consent to this or when it is necessary and or required to by law. The surgery is party to a number of information sharing agreements which are drawn up to ensure information is shared in a way that complies with relevant legislation.
How long do we keep your information for?
There are different retention schedules for different types of information and types of record. In the NHS, all commissioners and providers apply retention schedules in accordance with the NHS Records Management Code of Practice.
NHS data are subject to legal retention periods and should not be destroyed unless specific instructions to do so has been determined and received from the Data Controller.
What rights do I have?
By law you have certain rights related to your information. These are:
|
The right to be informed
|
You have the right to know what information that we hold about you, what we do with it and why. We inform patients through this privacy notice.
|
|
The right of access
|
You have the right to have a copy of the information that we hold on you. We must provide this to you within one calendar month and free of charge unless an exemption applies. We may need you to prove your identity before we can release any information to you.
|
|
The right of rectification
|
You have the right to have your personal data corrected if inaccurate.
|
|
The right to erasure
|
You have the right to have your personal data erased in certain circumstances.
|
|
The right to restrict processing
|
You have the right to restrict the processing of your personal data in certain circumstances.
|
|
The right to data portability
|
You have the right allows you to obtain and reuse your information for your own purposes. You have the right to have your information in a digital format.
|
|
The right to object
|
You have the right to prevent processing of your information in certain circumstances.
|
|
Rights related to automated decision making and profiling
|
We must inform you if we do this kind of processing, and offer you a human based alternative.
|
If you wish to exercise any of your rights, you can make contact by using the information below:
The Peninsula Practice
Mill Hoo
Alderton
Woodbridge
Suffolk
IP12 3DA
peninsula.practice@nhs.net
Telephone – 01394 411641
Practice Manager – Kay Goodchild-Critchley
Caldicott Guardian – Dr Lindsey Crockett
Your Data Matters
Information about your health and care helps us to improve your individual care, speed up diagnosis, plan your local services and research new treatments. In May 2018, the strict rules about how this data can and cannot be used were strengthened. The NHS is committed to keeping patient information safe and always being clear about how it is used.
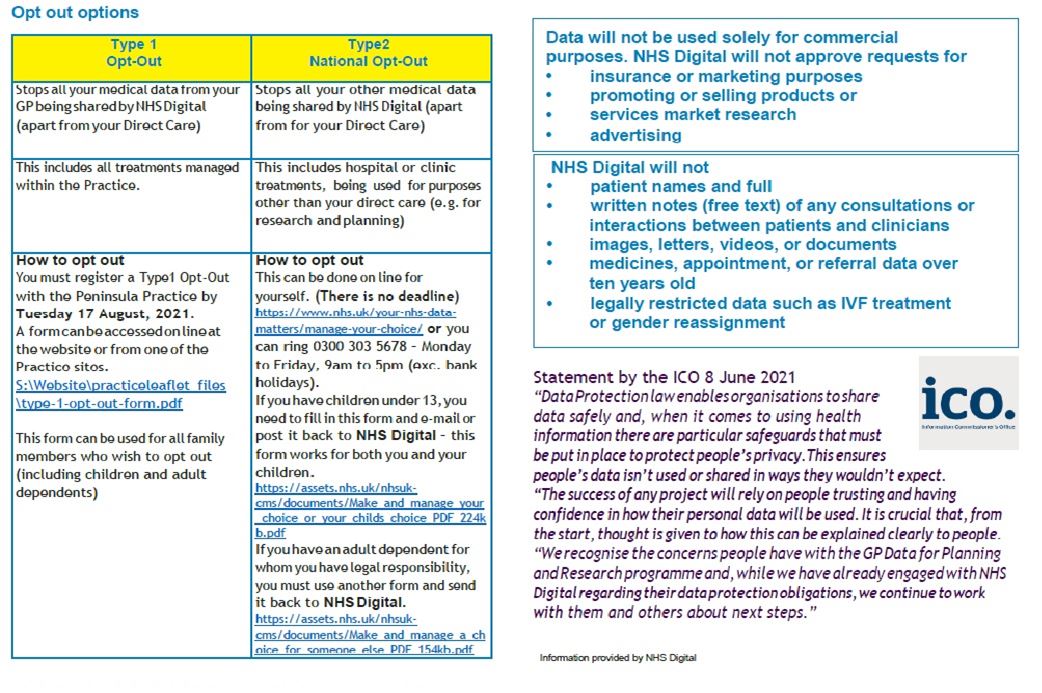
The National Data Opt-Out programme is a service that allows patients to opt out of their confidential patient information being used for research and planning.
Patients can view or change their national data opt-out choice at any time by using the online service at www.nhs.uk/your-nhs-data-matters.
Raising concerns
If you are concerned about the way we are handling your information or wish to make a complaint please contact the Practice Manager on 01394 411641.
If you still have further concerns then please contact the Data Protection Officer – Paul Cook – email: support@sneeicbdpo.freshdesk.com
The Data Protection Officer service is provided by Suffolk and North East Essex Integrated Care Board.
If the issue cannot be resolved by our organisation or the Data Protection Officer, you have the right to report it to the Information Commissioners Office (ICO). The ICO is the UK’s independent authority set up to uphold information rights in the public interest, promoting openness by public bodies and data privacy for individuals. You can contact them on the details below:
www.ico.org.uk/concerns/
Phone – 0303 123 1113
Customer Contact
Information Commissioner's Office
Wycliffe House
Water Lane
Wilmslow
SK9 5AF